By Arnold Ageta
Key facts
- Menopause is one point in a continuum of life stages for women and marks the end of their reproductive years. After menopause, a woman cannot become pregnant, except in rare cases when specialized fertility treatments are used.
- Most women experience menopause between the ages of 45 and 55 years as a natural part of biological ageing.
- Menopause is caused by the loss of ovarian follicular function and a decline in circulating blood oestrogen levels.
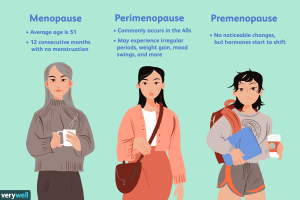
- The menopausal transition can be gradual, usually beginning with changes in the menstrual cycle. ‘Perimenopause’ refers to the period from when these signs are first observed and ends one year after the final menstrual period.
- Perimenopause can last several years and can affect physical, emotional, mental and social well-being.
- A variety of non-hormonal and hormonal interventions can help alleviate perimenopausal symptoms.
- Menopause can be a consequence of surgical or medical procedures.
How menopause occurs
For most women, menopause is marked by the end of monthly menstruation (also known as a menstrual period or ‘period’) due to loss of ovarian follicular function. This means that the ovaries stop releasing eggs for fertilisation.
The regularity and length of the menstrual cycle varies across a woman’s reproductive life span, but the age at which natural menopause occurs is generally between 45 and 55 years for women worldwide.
Natural menopause is deemed to have occurred after 12 consecutive months without menstruation for which there is no other obvious physiological or pathological cause and in the absence of clinical intervention.
Some women experience menopause earlier (before 40 years of age). This ‘premature menopause’ may be because of certain chromosomal abnormalities, autoimmune disorders, or other unknown causes.
It is not possible to predict when an individual woman will experience menopause, although there are associations between the age at menopause and certain demographic, health, and genetic factors.
Menopause can also be induced as a consequence of surgical procedures that involve removal of both ovaries or medical interventions that cause cessation of ovarian function (for example radiation therapy or chemotherapy).
Many women have already stopped menstruating before menopause, for example those who have had certain surgical procedures (hysterectomy or surgical removal of their uterine lining) as well as those using certain hormonal contraceptives and other medicines that cause infrequent or absent periods. They may still experience other changes related to the menopausal transition.
Changes associated with menopause
The hormonal changes associated with menopause can affect physical, emotional, mental, and social well-being. The symptoms experienced during and following the menopausal transition vary substantially from person to person. Some have few if any symptoms. For others, symptoms can be severe and affect daily activities and quality of life. Some can experience symptoms for several years.
Symptoms associated with menopause include:
- hot flushes and night sweats. Hot flushes refer to a sudden feeling of heat in the face, neck and chest, often accompanied by flushing of the skin, perspiration (sweating), palpitations, and acute feelings of physical discomfort which can last several minutes;
- changes in the regularity and flow of the menstrual cycle, culminating in cessation of menstruation;
- vaginal dryness, pain during sexual intercourse and incontinence;
- difficulty sleeping/insomnia; and
- changes in mood, depression, and/or anxiety.
Body composition and cardiovascular risk can also be affected. Women’s advantage over men in terms of cardiovascular disease gradually disappears with the significant decline in oestrogen levels after menopause. Menopause can also result in the weakening of the pelvic support structures, increasing the risk of pelvic organ prolapse. Loss of bone density at menopause is a significant contributor to higher rates of osteoporosis and fractures.
There are a variety of non-hormonal and hormonal interventions that can help alleviate symptoms of menopause. Symptoms that impact on health and well-being should be discussed with a health-care provider to identify available management options, with consideration of medical history, values, and preferences.
Pregnancy is still possible during perimenopause. Contraception is recommended to avoid unintended pregnancy until after 12 consecutive months without menstruation. Pregnancy after menopause is unlikely without fertility treatment that involves the use of donor eggs or previously frozen embryos.
During perimenopause and following menopause, it is still possible to acquire sexually-transmitted infections (STIs), including HIV, through unprotected sexual contact, including oral, anal, and vaginal sex. The thinning of the vaginal wall after menopause increases the chances of lesions and tears, thereby increasing the risk of HIV transmission during vaginal sex.
The importance of understanding menopause
It is critical to see menopause as just one point in a continuum of life stages. A woman’s health status entering the perimenopausal period will largely be determined by prior health and reproductive history, lifestyle and environmental factors. Perimenopausal and postmenopausal symptoms can be disruptive to personal and professional lives, and changes associated with menopause will affect a woman’s health as she ages. Therefore, perimenopausal care plays an important role in the promotion of healthy ageing and quality of life.
Menopause can be an important transition from a social perspective, as well as a biological one. Socially, a women’s experience of menopause may be influenced by gender norms, familial and sociocultural factors, including how female ageing and the menopausal transition are viewed in her culture.
The global population of postmenopausal women is growing. In 2021, women aged 50 and over accounted for 26% of all women and girls globally. This was up from 22% 10 years earlier. Additionally, women are living longer. Globally, a woman aged 60 years in 2019 could expect to live on average another 21 years.
Menopause can offer an important opportunity to reassess one’s health, lifestyle, and goals.

Public health challenges related to menopause
Perimenopausal women need access to quality health services and communities and systems that can support them. Unfortunately, both awareness and access to menopause-related information and services remain a significant challenge in most countries. Menopause is often not discussed within families, communities, workplaces, or health-care settings.
Women may not know that symptoms they experience are related to menopause, or that there are counselling and treatment options that can help alleviate discomfort. Those experiencing menopausal symptoms may feel embarrassed or ashamed to draw attention to their experiences and ask for support.
Health-care providers may not be trained to recognize perimenopausal and post-menopausal symptoms and counsel patients on treatment options and staying healthy after the menopausal transition. Menopause currently receives limited attention in the training curricula for many health-care workers.
The sexual well-being of menopausal women is overlooked in many countries. This means that common gynaecological effects of menopause, including vaginal dryness and pain during intercourse, may go unaddressed. Similarly, older women may not consider themselves at risk of sexually transmitted infections, including HIV, or may not be counselled by their providers to practice safer sex or get tested.
Many governments do not have health polices and financing for the inclusion of menopause-related diagnosis, counselling, and treatment services as part of their routinely available services. Menopause-related services are a particular challenge in settings where there are often other urgent and competing priorities for health funding.
WHO response
WHO considers that social, psychological and physical health support during the menopausal transition and after menopause should be an integral part of health care. WHO is committed to increasing understanding of menopause by:
- raising awareness of menopause and its impact on women at individual and societal levels, as well as on countries’ health and socioeconomic development;
- advocating for the inclusion of diagnosis, treatment and counselling related to management of menopausal symptoms as part of universal health coverage;
- promoting the inclusion of training on menopause and treatment options in pre-service curricula for health workers; and
- emphasizing a life course approach to health and well-being (including sexual health and well-being), by ensuring that women have access to appropriate health information and services to promote healthy ageing and a high quality of life before, during and after menopause.



One thought on “Breaking the Silence: Menopause Matters, and Here’s Why”